Introduction
Defined as activation of the pancreatic enzyme resulting in autolysis of the gland.
It is important to investigate for the possible causes of Acute pancreatitis before labeling it as 'idiopathic'.
Possible aetiology of Acute pancreatitis :
Gall stones
Alcoholism
Post ERCP
Abdominal trauma
Complication of cardiothoracic, biliary and abdominal surgery
Hypercalcemia
Hyperparathyroidism
Pancreatic Divisum
Autoimmune pancreatitis
Scorpion bite
Drugs : Corticosteroids, Azathioprine, Thiazide diuretics
Mumps, Cocksakie viral infection
Idiopathic
History
Both males and females are equally affected.
Age of onset is around 4th - 5th decade of life.
History of any gall stone diseases, or alcoholism is important (2 most important cause)
Though rare, but ask for recent contact with children with mumps or cocksakie infection.
Symptoms are usually triggered after consumption of large meal or alcohol.
Patient usually complains of sudden onset of severe, continuous epigastric pain, which typically radiates to the back, relieved by bending forwards.
It's accompanied by excessive vomiting and retching, with persistent nausea in between.
Breathing and movements exacerbates the pain.
General examination
Patient appears ill, with shallow breathing.
If the patient looks pale, diaphoretic, it is likely that it has complicated as a hypovolemic shock.
There might be mildly tinged jaundice if the pancreatitis is caused by gall stones.
Even 2-3 days after the illness, the mild tinged jaundice can be caused by compression of biliary duct by edematous head of pancreas.
Shock features of tachycardia, hypotension.
Low grade fever may or may not present.
Abdominal examination
In acute pancreatitis, the complains of the patient may indicate severe pain, but there is usually minimal findings
during abdominal examination.
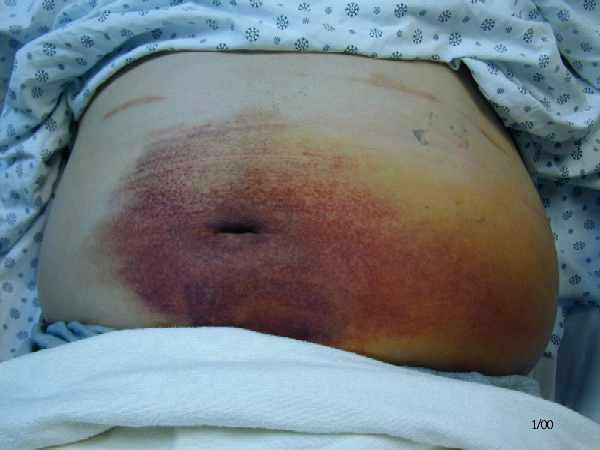
Cullen's sign
Grey Turner's sign
On inspection, if there's haemorrhagic pancreatits, there might be bruising (bluish purplish) discolouration over around the umbilicus (Cullen's sign) or left flank (Grey Turner's sign).
However, these signs are rarely seen nowadays.
The abdomen may not rise and fall with respiration, since the musculature is tightly contracted, and during onset of paralytic ileus.
Often there is accumulation of inflammatory exudates within the lesser sac, which eventually forms pseudocyst, suggested by epigastric fullness (distension), dullness during percussion over it.
Shifting dullness may be present, bowel sound may be reduced if there is pancreatic ascites.
Invesitgations
Acute pancreatitis is usually diagnosed by typical clinical presentation and laboratory investigation that reveals elevated serum amylase level. Serum amylase of 3-4 times greater than the normal level is suggestive of pancreatitis.
However, if serum lipase assay is available, it is more sensitive and specific.
Note that normal serum amylase level doesn't rule out Acute pancreatitis, and the level poorly correlates with the severity.
Both Ranson's and Glasgow's criteria is used to grade the severity of Acute pancreatitis.
If 3 or more factors are present in the patient, it indicates severe pancreatitis.
Imaging studies
Chest X ray, and plain abdominal X ray is not very helpful in the diagnosis of Acute pancreatitis
During early stages, if abdominal X ray is taken, non-specific signs such as Sentinel loop, Renal Halo sign or Colon cut off sign may be present.
Sentinel loop
Colon cut-off sign
Chest X ray may reveal pleural effusion, or if there is diffuse alveolar infiltrates, indicates ARDS.
Though Abdominal USG is non-diagnostic for Acute pancreatitis, but it must be done within 24 hours of presentation.
This is to rule out Acute cholecystitis as a differential diagnosis, to check whether the bile duct is dilated and to reveal any stones within the CBD (gall stone as a cause of Pancreatitis)
CT abdomen is not indicated in every patient.
Only when :
1) Diagnostic uncertainty
2) Severe pancreatitis
3) Clinical deterioration, with multi-organ failure, sepsis
4) Local complications occurs
Complications
Pancreatic pseudocyst
Management
a) Conservative
1) Gain IV access and rapid fluid resuscitation.
2) Give analgesics (usually IM pethidine is given)
3) Nil by mouth
4) Insertion of NG tube to relieve vomiting
5) Enteral feeding - nasojejunal tube (to maintain adequate nutrition)
6) Urinary catheterization is done
7) Monitor pulse, BP, urine output and CVP
8) Give antibiotics to prevent secondary infection
b) Endoscopic
If gall stone is strongly suspected as the cause of pancreatitis, the stones should be removed by basket (dormia) through endoscopic sphincterotomy.
If there is severe pancreatitis, or cholangitis occurs, both sphinterotomy and ERCP is done.
c) Surgery
Only indicated if : clinical deterioration during conservative management, unsure diagnosis, local complication occurs.
Adenocarcinoma of Pancreas
More common in males.
Age of presentation - 55-75 years old
85% of CA pancreas involves the head of pancreas, where the prognosis is usually poor.
Patients usually dies within 1 year of diagnosis (5 year survival is exceptional)
Upon presentation, most have progressed to a surgically incurable stage.
Though uncommon, but tumour arising from the distal CBD, duodenum and ampulla has a better outlook.
Currently, the risk factor of developing CA pancreas is thought to be :
Cigarette smoking
High fat and protein diet
Clinical features
Any elderly patient presents with painless jaundice, always suspect the possibility of Pancreatic cancer.
Typical symptoms are usually : Abdominal pain, jaundice and weight loss.
Jaundice is usually obstructive in nature, suggested by the classical triad of pruritus, clay-coloured stool and tea-coloured urine.
There might be steatorrhoea.
Abdominal pain - constant, dull aching, discomfort, over the epigastric region
Sought for symptoms of metastases
On examination, the gall bladder may be palpable, as accordance to the Curviosier's law, which states that,
"For patients presenting with clinically evident jaundice, and on examination the gall bladder is palpable, the cause is more likely to be due to Carcinoma of the Head of Pancreas".
Look for scleral icterus, hepatomegaly, etc.
Investigations
If stool occult blood test is positive, suggestive of a ampullary tumour.
Abdominal USG - usually done to look for liver metastases, or any mass lesion over the pancreas, and dilated bile ducts
CT abdomen - extent of metastases
To confirm the nature of obstruction, MRCP is preferred over ERCP since the former is less invasive.
Surgery of choice : Whipple's procedure








Very well written and informative article, thank you :-)
ReplyDeleteToshiba PVT-375BT
tq very much. very informative. it is unfortunate this blog is no longer active.
ReplyDeleteWhite Rock Laser Clinic has established a dominant position in the market by offering a wide range of services such wrinkles removal, birth marks, body hair removal, age spots removal,Wart and skin, Veins removal and much more. We have occupied the market by creating a powerful brand and large customer base through delivering reliable and healthy cosmetic treatments.
ReplyDeleteI am 29 years old and have been diagnosed with breast cancer, ease of treatment and a similar story, except for my first acceptance as a rejection of herbal medicine. I was not part of the Perseid movement and did not really build relationships with any of them, I just believed in their operation. I say this because it was during the use of Dr. Itua herbal medicine that I now attest that herbal medicine is real, the phytotherapy Dr. Itua heal my breast cancer which I suffered for 2 years. Dr. Itua herbal medicine is made of natural herbs, with no side effects, and easy to drink. If you have the same breast cancer or any type of human illness, including HIV / AIDS, herpes cancer,Ovarian Cancer,Pancratics cancers, bladder cancer, bladder cancer, prostate cancer, Glaucoma., Cataracts,Macular degeneration,Cardiovascular disease,Autism,Lung disease.Enlarged prostate,Osteoporosis.Alzheimer's disease,psoriasis ,Tach Diseases,
ReplyDeleteDementia.kidney cancer, lung cancer, skin cancer, skin cancer and skin cancer.testicular Cancer, , LEUKEMIA, VIRUSES, HEPATITIS, INFERTILITY WOMEN / MAN, LOT OF LOVE, LOTTERY. ITS CONTACT EMAIL / WHATSAPP: info@drituaherbalcenter.com Or drituaherbalcenter@gmail.com/ +2348149277967
Here is my contact phone number. +1-913-9518-145 if you would need some advise from me.
It is no secret that I have a very deep and personal relationship with God. I have pushed and resisted that relationship this past year through all the bullshit I have had to go through living with Herpes but once again, God is bigger than my stubbornness and broke through that outbreak cold sore and all I had Genital Herpes. For me personally, hearing over and over how I am not good enough has really invaded my mind in the worst way possible. I completely shut down and I was just waking up like is this how life going to end this temporary herpes outbreak “fuck everybody with herpes if you know what I mean” but let's be honest here...
ReplyDeleteIt is cowardly to say no to herbal medicine. It is fear based. And it is dishonest to what my heart wants. Don't build a wall around yourself because you are afraid of herbals made or taking a bold step especially when it's come to health issues and getting cured. So many young men/ women tell me over and over that Dr Itua is going to scam me but I give him a try to today I feel like no one will ever convince me about herbal medicine I accept Dr Itua herbal medicine because it's cure my herpes just two weeks of drinking it and i have been living for a year and months now I experience outbreak no more, You can contact him if you need his herbal medicine for any such diseases like, Herpes, Parkinson, Diabetes, Hepatitis, Syndrome, Cancers, HIV, Epilepsy, Infertility, and any kind of disease & Infections Love Spell,. Email..drituaherbalcenter@gmail.com then what's app.+2348149277967.... My advice to any sick men/women out there is simple... Be Always an open book. Be gut wrenching, honest about yourself, your situation, and what you are all about. Don't hold anything back. Holding back will get you nowhere...maybe a one way ticket to lonelyville and that is NOT somewhere you want to be. So my final truth...and I'm just starting to grasp this one..
I want to share with you all on how Dr Itua saves my life with his powerful Herbal medicines, I was diagnosed of Oral/Ovarian Cancer which i suffered from for 5 years with no positive treatment until when My son came to me in the hospital when i was laying down on my dying bed waiting for god to call out my name to join him in heaven.
ReplyDeleteMy son was so excited that very day he came across Dr Itua on Blogspot, we decided to give him a try although we Americans are so scared to trust Africans but i really have no choice that time to choose life in between so we gave a try to Dr Itua Herbal medicines, god willing he was a good man with a god gift. Dr Itua sent us the herbal medicine. It was three bottles. I take it for a three weeks instructor and these herbal medicines heal me, cure my Oral/Ovarian Cancer completely. I have been living for 9 months now with a healthy life with no more symptoms.
I'm sponsoring Dr Itua in LA Advert on Cancer patent seminar which my son will be participating too and other patent Dr Itua has cured from all kind of human disease, also if you are sick from disease like,Epilepsy,Breast Cancer,Prostate Cancer,Throat cancer,Thyroid Cancer,Uterine cancer,Fibroid,Angiopathy, Ataxia,Arthritis,Brain cancer,Hiv,. Vaginal cancer,Herpes,Colon-Rectal Cancer,Chronic Disease.Amyotrophic Lateral Sclerosis,Brain Tumor,Fibromyalgia,Fluoroquinolone Toxicity,Multiple myeloma,Tach Diseases,Leukemia,Liver cancer,
Esophageal cancer,Gallbladder cancer,,Bladder cancer,Gestational trophoblastic disease,Head and neck cancer,Hodgkin lymphoma
Intestinal cancer,Kidney cancer,Hpv,Lung cancer,Adrenal cancer.Bile duct cancer,Bone cancer,Melanoma,Mesothelioma,Neuroendocrine tumors
Non-Hodgkin lymphoma,Cervical Cancer,Oral cancer,Hepatitis,Skin cancer,Soft tissue sarcoma,Spinal cancer,Pancreatic Cancer, Stomach cancer
Testicular cancer,
Syndrome Fibrodysplasia Ossificans ProgresS sclerosis,Alzheimer's disease,Chronic Diarrhea,Copd,Parkinson,Als,Adrenocortical carcinoma Infectious mononucleosis,Vulvar cancer,Ovarian cancer,,Sinus cancer, Here Is The Wonderful Healer Contact. Name_ Doctor Itua, Email Contact: drituaherbalcenter@gmail.com, Phone/WhatsApp: +2348149277967
If you're seeking effective homeopathic care for Acute Pancreatitis in Hyderabad, look no further than "The Art Of Homeopathy." Renowned for its holistic approach to healing, this establishment offers top-notch treatment under the guidance of experienced homeopathic practitioners. With a focus on addressing the root causes of ailments, they tailor their remedies to individual needs, ensuring a personalized and comprehensive healing journey for each patient. "The Art Of Homeopathy" in Hyderabad stands out as a trusted destination for those seeking natural and well-rounded solutions for Acute Pancreatitis and various other health concerns.
ReplyDelete