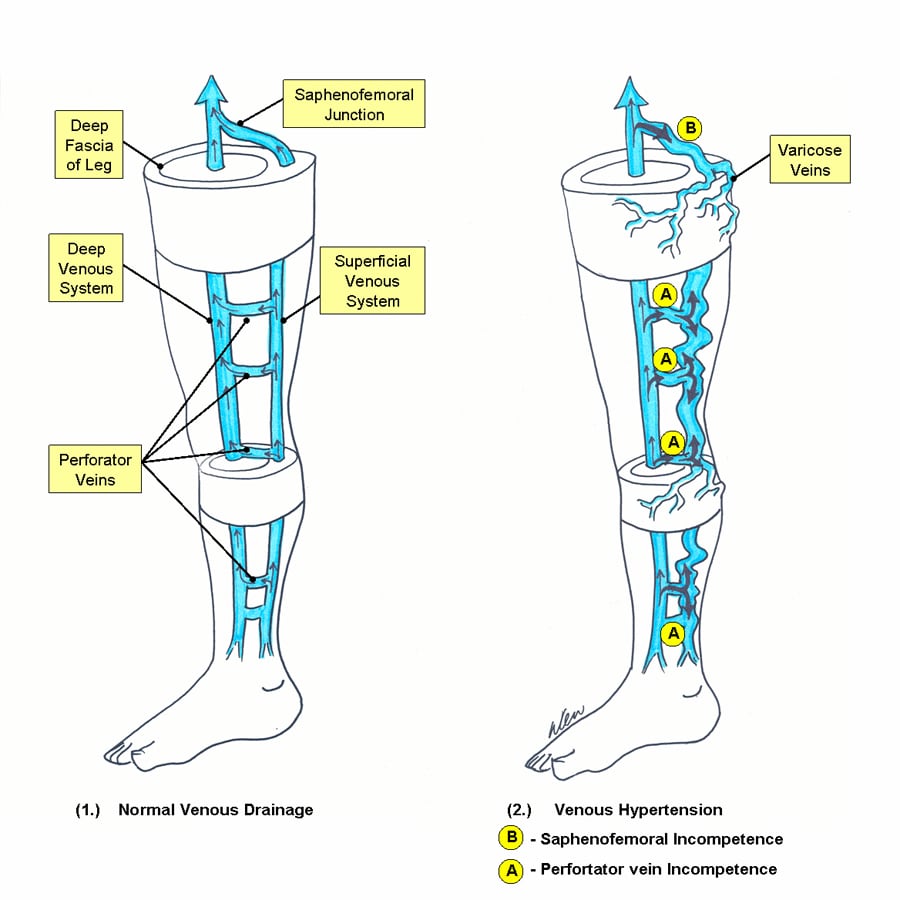
The venous system of the lower limb is divided into the superficial and deep system. The superficial system comprises of
a) Long saphenous veins
b) Short saphenous veins
Long saphenous veins
It begins from the medial end of dorsal venous arch, ascending in front of the medial malleolus, then along the medial aspect of the leg and knee, anteriorly along the thigh, finally pierces the cribiform fascia and joins with the femoral vein at the SF junction (located 4cm lateral and below of the pubic tubercle)
Tributaries :
1) In the leg - anterior and posterior arch veins
2) In the thigh - medial and lateral thigh veins
3) At the SF junction - superficial circumflex iliac, superficial inferior epigastric, and superficial external pudendal
Short saphenos vein
It begins from the lateral end of dorsal venous arch, ascends behind lateral malleolus, then towards the popliteal fossa, where it pierces the popliteal fascia and joins the popliteal vein
Perforators
These are communicating veins, that pierces the deep fascia, ensures unidirectional flow of blood from the superficial to the deep system. Note that all veins of the lower limb are equipped with venous valves to prevent backflow of blood.
The constant perforators for the long saphenous system : (4 in the leg + 1 in thigh)
a) Crockett's perforators : 3 in number, located 5cm, 10cm and 15cm above the tip of medial malleolus
b) Boyd's perforator : Single, located below the knee
c) Dodd's perforator : Single, located at the level of mid-thigh
There is only one constant perforator for the short saphenous system, which is located 10cm above the lateral malleolus.
The deep system comprises of :
Each artery of the lower limb, namely the anterior, posterior, and lateral tibial artery, is accompanied by 2 veins (known as vena comitantes). Hence, all the 6 veins join just below the popliteal fossa to form the popliteal vein, and becomes the superficial femoral vein as it passes through the hunterian's canal. Finally, as it joins with the deep femoral vein at the upper thigh, it forms the femoral vein.
Thread veins
These are small veins, with diameter of 1-2mm, appears reddish, bluish or purplish, and is usually asymptommatic (only cosmetically disfiguring). However, it might be an indicator of an underlying muscle pump failure, and varicose veins might develops in the future.
Physiology
The calf muscles act as a pump, which ensures blood flow from superficial to deep system, and ascending upwards in the deep system.
However, this is only possible when there're competent venous valves.
Varicose veins
Defined as dilated, tortous, and elongated superficial veins of the lower limbs.
Usually secondary to chronic venous hypertension.
Pathophysiology :
1) More common in females
2) Occupation involving long hours of standing (policeman, conductors) are at risk of developing such conditions, due to chronic pooling of blood within these leg veins -> dilatation of these veins -> valvular incompetence
3) Pregnancy : Risk of developing varicosities increases, due to progresterone mediated venodilatation and the pressuring effect of the enlarging fetus to the inferior vena cava
4) In cases of post-thrombotic veins, where there's valvular damange, it causes reversal of blood flow
5) In cases of intravascular clotting (DVT) or extrinsic compression of the veins (eg, pelvic tumours), causing elevated venous pressure.
6) Lastly, primary varicosities seems to run in family.
Classification
1) Primary varicose veins
Due to unknown etiology
Probably due to inherited/congenital weakness of the vessel wall or even absence of venous valves
2) Secondary causes
Might developed due to valvular destruction (secondary to venous thrombosis)
Pregnancy
Ovarian cyst/Fibroids
Pelvic cancers
Abdominal lymphadenopathy
Iliac vein thrombosis
Ascites
Retroperitoneal fibrosis
Important points in History taking :
1) During early phase of disease, symptoms are usually subjective :
Aching, dragging pain over the calf region
Burning sensation felt over the calf
Later followed by some skin changes (explained later)
2) Occupational history as mentioned above is important
3) Any family history of varicose vein
4) Any previous h/o of deep vein thrombosis
5) Any h/o of pregnancy, or even pelvic tumours
6) Any h/o of complications (ulcers, haemorrhage, ruptures, DVT, superficial thrombophlebitis)
On examination :
1) Make sure that you're examining the patient while he/she is standing
2) Inspect for any varicosities along the region of long and short saphenous veins
3) Inspect for any saphena varix at the upper end of the long saphenous vein (ask the patient to cough to appreciate any cough impulse and feel for a palpable thrill)
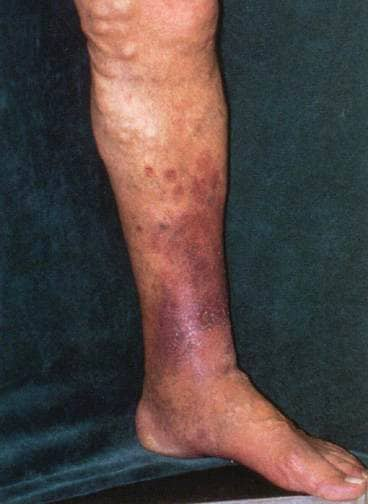
4) Look for complications :
a) Eczema and dermatitis : Due to chronic irritation secondary to RBC breakdown (hemosiderin deposition)
b) Lipodermatosclerosis : Thickening and induration of the pigmented skin of lower leg due to replacement of the subcutaneous fat with fibrous tissue.
c) Varicose ulcers
More common in females
Responsible for about 2/3 cases of leg ulcers
Located above medial malleolus (long saphenous system)
Located above lateral malleolus (short saphenous system)
Slopping edge, with unhealthy granulation tissue seen over the floor
Skin edges surrounded by pigmentation
d) Marjolin's ulcer
A type of squamous cell carcinoma developed due to excessive scarring of tissue, secondary to chronic venous ulcer (in this case)
There's extensive damage to the surrounding lymphatic vessels and vascular channels. Hence, there's no way for this malignant lesion to spread to distant areas.
Besides, it's radio and chemo-resistant
The only way of treatment is to peform wide-excision + extensive skin grafting.
e) Superficial thrombophlebitis
Due to inflammation of the superficial veins (red and tender cord)
Various specific test for varicose veins :

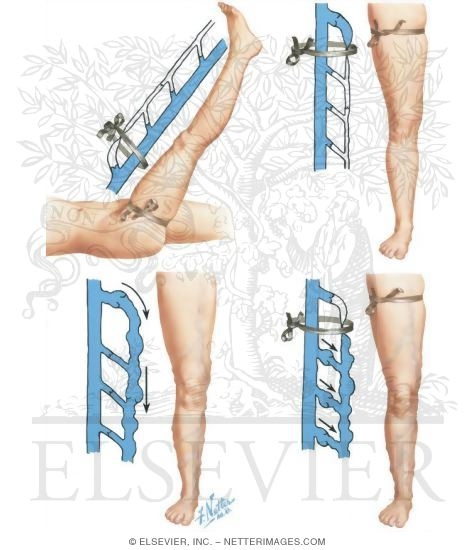




The vein treatment can improve the overall appearance of a person and how they are perceived by others to give more confidence.
ReplyDeleteveins
Thank you so much for sharing this wonderful and informative blog to us. Many people will be more aware now and that is because they have read your article. My Center for venous disease clinic agrees on all the information you have shared here. Keep blogging.
ReplyDeleteOh my word! This just look painful. How does this disease come about exactly? I really hope that there are ways to prevent it from happening. My grandmother had been suffering from this condition for a little while and has been going to treatments to help her get through it. I'm glad we have ways to treat varicose veins.
ReplyDeleteThanks for sharing. Varicose veins are quite painful & i personally recommend minimal invasive treatments are better for varicose veins. One of my cousin used to suffer with varicose veins then she moved for minimal invasive treatment by Dr. Abhilash at http://www.interventionsinradiology.com/. With in minimal recovery time she was completely cured.
ReplyDeleteHi Fusionclk
ReplyDeleteThanks for sharing varicose veins post.You have mention varicose veins post in detail. I think it's a very informative to all varicose veins patient. But don't try firstly discuss to Dr. Jawdat Abboud. He is varicose veins specialist in U.S.A
Stop suffer from varicose in just one week, naturally. http://bit.ly/1RydBWN
ReplyDeleteThis is all very good information. Have you found if surgical vein removal or natural remedies have been more effective in terms of long-term solutions for you?
ReplyDelete- Dr. Thomas S. Parisi, Las Vegas Vein
This is all very good information. Have you found if surgical vein removal or natural remedies have been more effective in terms of long-term solutions for you?
ReplyDelete- Dr. Thomas S. Parisi, Las Vegas Vein
White Rock Laser Clinic has established a dominant position in the market by offering a wide range of services such wrinkles removal, age spots removal,Veins removal and much more. We have occupied the market by creating a powerful brand and large customer base through delivering reliable and healthy cosmetic treatments.
ReplyDeleteINFORMATIVE POSTS:There are numerous acne scar treatments in Abu Dhabi & Dubai that help people get rid of these scars that result from chronic acne and damage the appearance.
ReplyDeleteWe also provide the best treatment of acne so just visit our site and get the special discount visit on… Acne Treatment in abu dhabi
Thanks for sharing these pictures. This should give me a better understanding.
ReplyDeleteVaricose Vein Treatment Chandler
This is an excellent article! The information here is extremely thorough, breaking down the different causes and symptoms etc. Actually I think this is the most substantial article I've seen on the subject so far. Since there is nothing here on potential solutions for varicose veins I thought I would offer my two cents. I can't say much for surgery however if anybody is looking for a natural solutions to your varicose vein problem check out my blog. http://bestalternativeremedy.com/
ReplyDeleteWhite Rock Laser Clinic has established a dominant position in the market by offering a wide range of services such wrinkles removal, age spots removal,Wart and skin, Veins removal and much more. We have occupied the market by creating a powerful brand and large customer base through delivering reliable and healthy cosmetic treatments.
ReplyDeleteYou all need to consult with the Dr. Mohan Singh who is the owner of the Mohan Skin Centre, if anyone from you wants to get the perfect varicose veins treatment in India with desired results. He is one of the best dermatologist in India having experience of more than 40 years.
ReplyDeleteWhite Rock Laser Clinic has established a dominant position in the market by offering a wide range of services such wrinkles removal, age spots removal,Wart and skin, Veins removal and much more. We have occupied the market by creating a powerful brand and large customer base through delivering reliable and healthy cosmetic treatments.
ReplyDeleteLooking for natural medicine to schizophrenia without any side effect Dr. Johnson is the best because is Medication has no side effect, After my son being diagnosed of Mania in 2010, I have used numerous medicine for him with no improvement. I remember him feeling abandoned and terrified of the many injection needles that seemed necessary to keep him calm. All Western Medicine used in the past did not have any noticeable difference,one day as i was going through the internet i came across so many people with different disease testifying about Dr Johnson herbal remedies,i ordered for it on line,that's when he started using Dr Johnson Herbal Medicine,and now is completely cured from Mania , his medicine is a permanent cure to Mania, for more info contact drjohnson958@gmail.com for advice and for his product
ReplyDeleteThis is the depiction of extreme cases. My cousin also had such kind of problem and he took Varicose veins surgery in India. Though the surgery get costy but the result is satisfying.
ReplyDeleteGreat Blog. Thanks for the information you have shared.
ReplyDeleteVaricose veins, commonly observed in legs, are enlarged tortuous veins that have lost their elasticity. A vein goes varicose when it’s valves are unable to prevent backflow, thus causing pooling of blood. Varicose veins are quite often a cosmetic concern, specially in women.
Healing Hands Clinic has state-of-the-art facilities to treat VARICOSE VEINS. The veins are treated with laser by a procedure called Endovenous Laser Ablation (EVLA). Dr Paresh Gandhi, VARICOSE VEINS expert at Healing Hands Clinic has successfully treated a large number of cases using EVLA technique.
Very Nice Article Vascular Care Center is a specialized medical organization for treatment of diseases related to vascular, endovascular blood vessels, arteries, and veins. Any stage of disease can be healed at Vascular Care Center by proficient Surgeons with utmost care and consultation. If the disease is in severe stage then doctors will suggest a surgery treatment. India's best Vascular Surgeon Dr.G.V. Praveen Kumar had done many Vascular and Endovascular surgeries.
ReplyDeleteVascular surgeon in Hyderabad
Wonderful blog!! you write the nice article for removal of varicose veins in Chicago. Thanks for sharing it.
ReplyDeleteHappiness is all i see now I never thought that I will be cured from HERPES virus again. I have been suffering from a deadly disease (HERPES) for the past 3 years now, I had spent a lot of money going from one places to another, from churches to churches, hospitals have been my home every day residence. Constant checks up have been my hobby not until this faithful day, I was searching through the internet, I saw a testimony on how Dr Ogudugu helped someone in curing his HERPES disease, quickly I copied his email which is greatogudugu@gmail.com just to give him a test I spoke to him, he asked me to do some certain things which I did, he told me that he is going to provide the herbal cure to me, which he did, then he asked me to go for medical checkup after some days after using the herbal cure, behold I was free from the deadly disease, he only asked me to post the testimony through the whole world, faithfully am doing it now, please brothers and sisters, he is great, I owe him in return. If you are having a similar problem just email him on ( greatogudugu@gmail.com ) or you can whatsApp his mobile number on +27663492930
ReplyDeleteRJM Herbal Care in Chennai, excels in Asthma Treatments no matter how severe, helping patients get a better life is the motto of RJM herbal care, there is a solution for other ailments concerning Skin and Piles related problems, Herbal methods are far more effective in terms of healing a patient with NO side effects.
ReplyDeleteTreatment of varicose veins . Thanks for sharing!
ReplyDeleteGreat Blog. Thanks for the information you have shared.
ReplyDeleteVaricose veins removal, but varicose veins commonly observed in legs, are enlarged tortuous veins that have lost their elasticity. A vein goes varicose when it’s valves are unable to prevent backflow, thus causing pooling of blood. Varicose veins are quite often a cosmetic concern, specially in women.
thanks for sharing; I have a fear about the medicle procedures of any kind. I know its not good but i want to know that Is massage good for varicose veins. kindly give your suggesion.
ReplyDeleteThanks for sharing this post with me. Ever saw swollen and apparent veins with blood? Yes, it is totally normal and there are no major health problems associated with it. Varicose veins removal treatment can be a good option for this problem.
ReplyDeleteLovely blog with much more interesting article, I will keep on reading your update. Thanks for the share
ReplyDeleteGynecologist in Bangalore | IVF Treatment Centre in Bangalore| Uterus Removal Surgery in Bangalore | Fibroids Surgery in Bangalore
Thanks for sharing such a valuable information it was very helpful
ReplyDeleteVaricose Veins Treatment Dubai
Thank you for discussing this very useful article. I heard something new from you. Keep blogging. varicose veins treatment in bandra
ReplyDeleteVaricose veins Clinic - Book Appointment Melbourne Varicose Veins, Most Reviewed Doctor and Clinic in Melbourne, Victoria, Australia, Spider Vein Treatment Specialist.
ReplyDeleteI have read a few of the articles on your website now, and I really like your style of blogging. I added it to my favorites blog site list and will be checking back soon. Please check out my site as well and let me know what you think. varicose and spider veins removal
ReplyDeleteI am very much pleased with the contents you have mentioned. I wanted to thank you for this great articlevaricose veins treatment dubai
ReplyDeleteHey thегe and Thank you so much for sharing this information. It has very useful. Please keep sharing.If you want more about the best treatment for varicose veins Kindly click the link
ReplyDeletevaricose veins specialist doctor in coimbatore
I was looking for these types of articles, Very helpful and informative. Thanks for sharing with us, want to know more about Varicose Veins Specialist in Coimbatore, Kindly visit the link.
ReplyDeleteThis is a very informative blog. keep up the good word, i fund a similar useful blog on varicosities treatment
ReplyDelete